What Pelvic Floor Dysfunction is, How it Happens, and How to Heal it
How Your Shoulders, Feet, and Nervous System Connect to Pelvic Floor Function
Though historians say that all roads lead to Rome, physical therapists say all roads lead to the pelvis. That is because the pelvis is connected to both the trunk and the legs, between the internal organs and the outside world. The pelvis is involved in:
Support: It provides a sturdy base for the spine, supports the weight of the upper body, and connects the upper body to the lower body.
Connection: Many major muscle groups including the quadriceps, hamstrings, gluteal muscles, abdominal muscles, psoas (which connects the upper bones of the low back, the lumbar spine, to the pelvis), quadratus lumborum (which connects the pelvis to the ribs), as well as other muscles that flex and extend the spine.
Organs: The pelvic floor supports the bladder, intestines, and internal reproductive organs (prostate for men and uterus, ovaries, and vagina for women)
Movement: Alignment and mobility of the pelvis has a significant impact on how well we can walk, run, and move more generally.
Childbirth: The pelvis is literally a portal from the otherworld to this world by bringing new life into the world.
Because of all of these connections, problems in the hands, feet, or emotions can have a big impact on the pelvis and likewise, problems in the pelvis can cause problems relatively far away. For example, I have been participating in a training program targeted on healing the pelvic floor and have noticed substantial improvement in chronic shoulder and calf injuries.
The pelvic floor is part of the canister that makes up your core, along with the diaphragm, abdominal, and back muscles. When the core is healthy, it can respond to the many varied and dynamic movements we need to engage in throughout the day. If you’ve ever dealt with stress incontinence, low back pain, or pelvic pain, you know that spontaneous movement without planning and strategy can be difficult. However, when the system functions well, it can respond to variable forces from many different directions. You can pick up a bag of dog food from the floor or lower baggage from the overhead compartment of an airplane. You can sneeze, bend and twist, or jump on a trampoline.
When the muscles of the pelvic floor are dysfunctional people may experience:
Difficulty starting urination
Bulging of the bladder or into the vagina, the uterus outside the vagina (uterine prolapse), the upper portion of the vagina outside the vagina (vaginal prolapse), the intestines into the vagina, or the rectum into the vagina
Involuntary leakage of urine (incontinence)
Pain during or after sexual intercourse
Constipation
Involuntary leakage of stool (fecal incontinence)
Pelvic pain
Pain where the pubic bones meet (pubic symphysis)
Pain where your tailbone meets your pelvis (sacroiliac joint)
Low back pain
Pelvic floor dysfunction affects 50% of childbearing women, and 1 in 5 women have surgery to address stress urinary incontinence (the type of incontinence caused by increased abdominal pressure like sneezing, coughing, jumping, and heavy lifting). Pelvic floor dysfunction is common and getting moreso. In 2010, there were 28 million American women with pelvic floor dysfunction. Researchers project that there will be 43-58 million women with pelvic floor dysfunction in 2050 and a 55% increase in both urinary and fecal incontinence over that time. Though pelvic floor dysfunction is more common in women who have had children, other factors like a sedentary lifestyle and stress mean that people who have never had children (including men) can experience pelvic floor problems. When women mention symptoms of pelvic floor dysfunction to a medical provider, they are often instructed to do kegels. Kegels are voluntary contractions of the pelvic floor muscles. However, pelvic floor weakness is not the only cause of pelvic floor dysfunction. Too much tension in the pelvic floor muscles or difficulty coordinating pelvic floor movements can also cause painful or troublesome symptoms. Kegels can worsen tension in already too tight pelvic floors.
Pelvic Floor Tension
Four main issues contribute to pelvic floor tension (though there are other less common ones).
High-intensity exercises like heavy lifting or box jumps: If you start lifting heavy without learning how to manage the increase in pressure inside your abdomen, sometimes the pelvic floor stops knowing when and how to relax.
Bathroom habits: Holding your pee frequently or for long durations can lead to overuse and tightness in pelvic muscles. Sitting on the toilet for a long time reading or scrolling can also overuse and tighten those muscles.
Stress and anxiety: Just like your jaw or shoulders tighten up when you’re under stress, your pelvic floor and gluteal muscles do too. We often have less sensory perception to notice it than we do in other muscle groups.
Injury due to childbirth: The pelvic floor often tightens in response to muscle tears or other traumas to protect you from further injury.
People with pelvic floor tension often experience two main issues–pain or problems with peeing and pooping. When the muscles in the front of the pelvic floor get too tight, it can be difficult to empty the bladder all the way, which increases the likelihood of developing UTIs. These tight pelvic floor muscles can also lead to muscle spasms. Those spasms prevent the urethra from opening enough to let urine out. When you push against the spasm, it can sometimes cause a feeling of burning when you pee, even though you don’t have an infection. When pelvic floor muscles are tight, they can also compress the bladder or other nearby structures which gives the urge to pee frequently. Additionally, incontinence either due to pressure (coughing, sneezing, laughing, lifting, jumping) or a strong urge to pee both suggest that the pelvic floor isn’t working as it should. Lastly, when the muscles at the back of the pelvic floor are too tight, they can cause problems with pooping, usually constipation or straining.
Several types of pain are associated with pelvic floor tightness. Just like muscular tightness around the urethra and anus affects our ability to pee and poop, tightness around the vagina can lead to painful sex. Tight pelvic floor muscles also frequently contribute to painful period cramps, pelvic pain, low back pain, hip pain, and tailbone pain. Tight pelvic floor muscles can also contribute to trigger points in the thighs, hips, back, and abdomen.
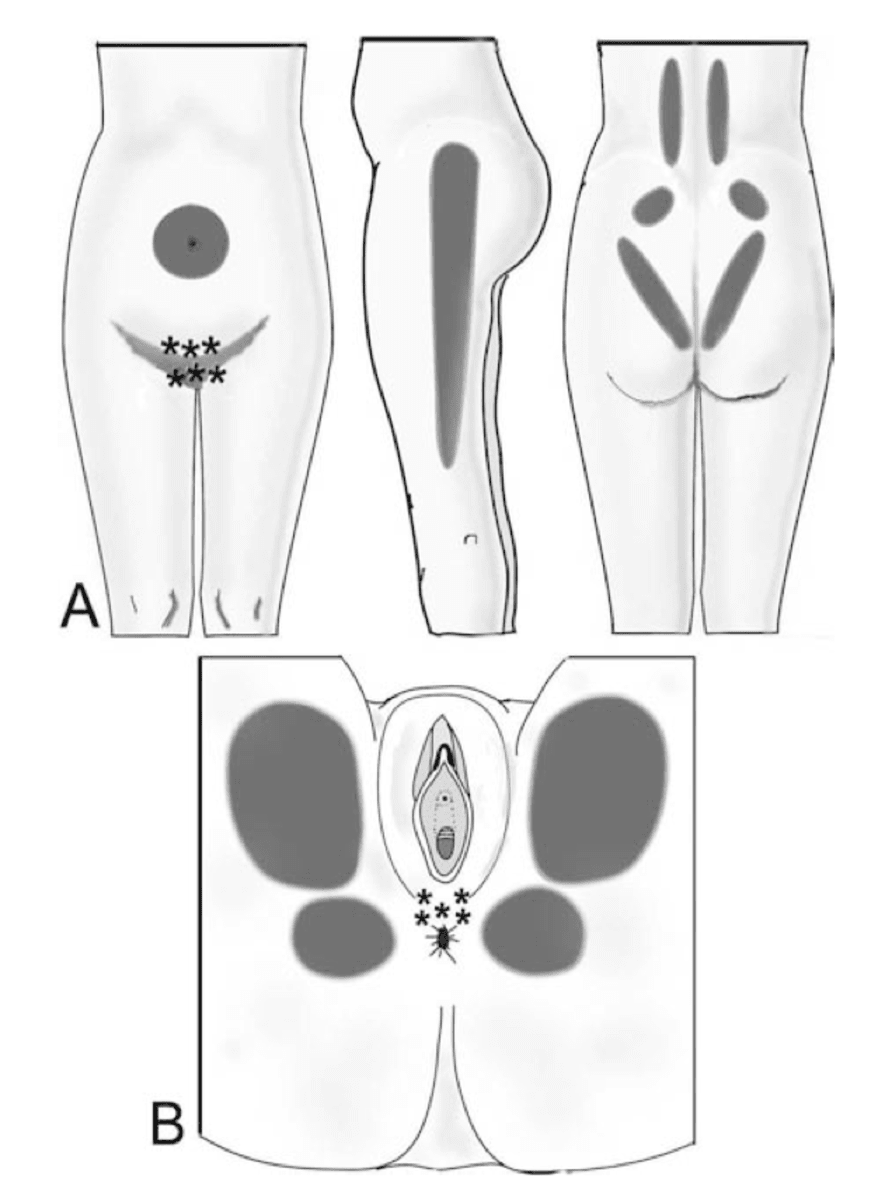
When we are under stress, our sympathetic nervous system activates. That causes increased tension in all of our muscles, including the pelvic floor. The pelvic floor muscles become tight and overactive, which leads to incontinence, pain with sex, and pelvic pain. In other words, the pelvic floor needs not only the strength to contract and the endurance to maintain that contraction, but also the length to be able to relax and release tension.
Pelvic Floor Weakness
Pregnancy, particularly accompanied by a long or difficult delivery is the most common, but certainly not the only, cause of pelvic floor weakness. The additional weight and pressure on the pelvic floor during pregnancy can stretch those muscles. Pelvic surgeries, getting older, and poor posture can contribute as well. It is often difficult to distinguish whether symptoms of pelvic floor dysfunction are due to weakness or excessive tension because they often involve pain and incontinence in both. Pelvic organ prolapse is more likely in people with weak pelvic floor muscles. Stress incontinence (peeing due to increased pressure like lifting, coughing, sneezing, jumping) is more likely due to pelvic floor weakness than tension. Urge incontinence, peeing because an urge comes suddenly is more likely due to pelvic floor tension, but both can happen from either.
Psoas Tightness
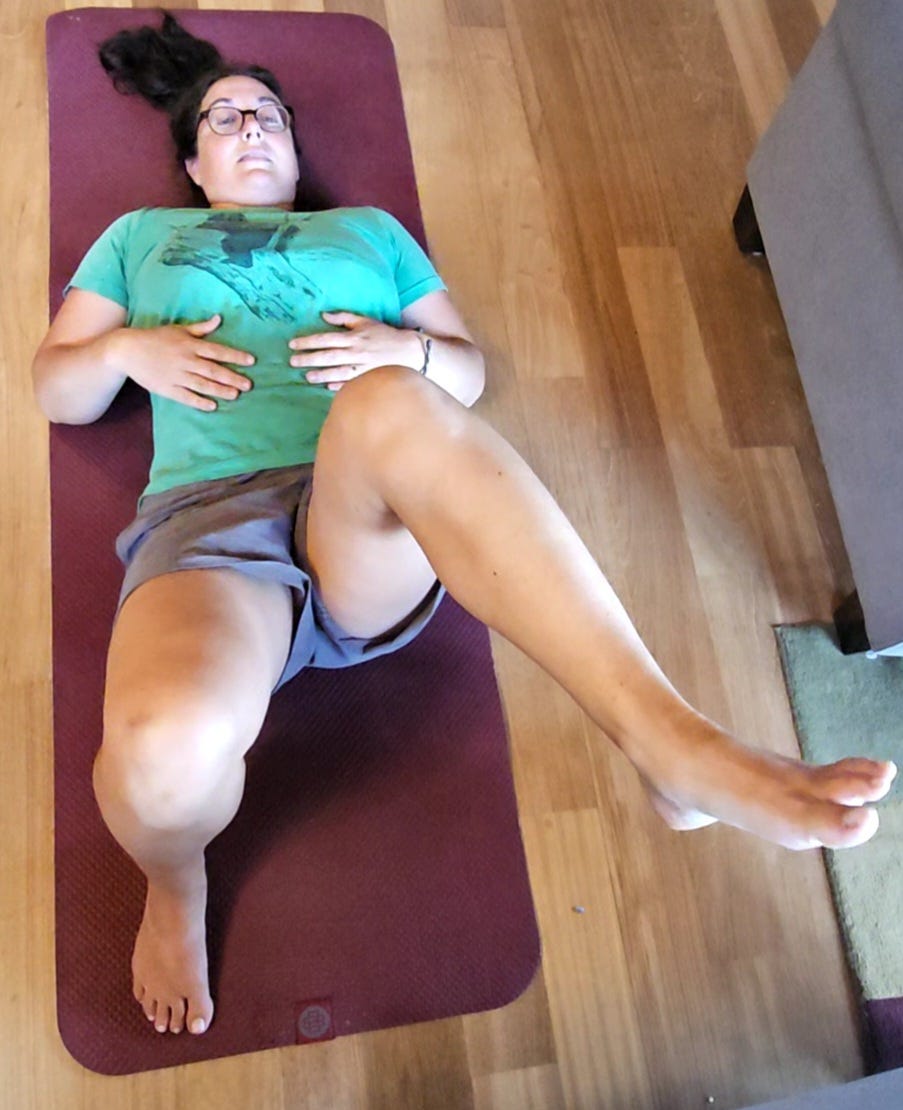
Many people have very tight psoas muscles. The most common cause is excessive sitting. Our bodies evolved to be mobile more than we are. Hunter-gatherers aren’t constantly moving though, they actually work less hours per day than we do. They also rest in different ways. The key is that almost every chair we sit in encourages us to sit with the pelvis tucked (sitting mostly on our tailbone). That requires less muscular effort than sitting so the weight is distributed over the triangle that includes the pubic bone and the sitting bones. Here is the difference in sitting positions:
Certainly, it is less effort to sit in the first way. That’s why we do it. However, you can also see how my shoulders slump forward when I do that. Over time, that creates a lot of unnecessary neck and shoulder tension too.
Here are some examples of chair-free resting positions from Nutritious Movement:
Additionally, many of us perform exercises that result in repetitive hip flexion like running, cycling, and weightlifting. The psoas is also known to store emotional tension.
A tight psoas muscle pulls on the spine and pelvis. It will pull the pelvis too far forward leading to pelvic floor weakness. A weak psoas muscle can’t stabilize the pelvis and will lead to worse posture that increases pressure on the pelvic floor.
Shoulders, Feet, and the Pelvic Floor
Anatomically, the pelvis and the shoulder are intimately connected. The abdominal oblique muscles connect the low back and pelvis to the opposite shoulder. The gluteus maximus muscle extends into the fascia of the low and mid-back which crosses over the latissimus dorsi (a large back muscle that is used for pulling things down or back). The tilt of the pelvis changes the curvature of the spine, which changes posture. The head of the humerus bone is positioned inappropriately when there is low back and pelvis dysfunction. Walking effectively depends on integration of the shoulder and pelvis. Not only that, but the pelvic floor engages before we move our shoulder every single time. Physical therapist,
notes, “The pelvic floor, along with the other inner Core components (Diaphragm, Transverse Abdominis, and Multifidus), secure our physical center to create a sturdy anchor for the muscles that support and create shoulder motion before we start moving our arm, every time we move our arm, no matter which way we move our arm.” Tight shoulders often pull us into poor posture. That along with a forward head position changes our breathing mechanics, restricts rib range of motion, and increases the pressure in the abdomen.Our feet impact pelvic health in several different directions. First, there are the biomechanical changes that depend on where and how your foot strikes the ground. Is it only your toes? Does your weight fall on your outer foot? Do your arch and knee collapse inward? Second, motor and sensory input from the foot and genitals are located next to each other in the brain. Third, Fascia connects from the foot to the spine and core muscles. Last, feet and pelves serve as shock absorbers for the body.
Flat feet/collapsed arches cause thigh and hip rotation, which can lead to excessive gripping and tightness in the pelvic floor. Rigid feet decrease the body’s ability to absorb impact, which increases pressure in the abdomen, especially during running. The nerves that supply the pelvic floor also supply the small muscles in the feet as well. Here are a couple of examples from OrthoPelvic PT:
For a person with flat feet/fallen arches:
While walking/running/existing, the knee falls in which pulls the adductors
This causes the hip to rotate in which pulls the rotators
Then tension from the knee/hip pulls on the pelvic floor muscles and put them in a tightened position
Tight pelvic floor muscles can cause the issues listed above.
For a person with high arches and a rigid/stiff foot
Stiffness in the foot means less force is absorbed when walking/running etc.
Because less force is absorbed by the foot, more force goes up to the pelvic floor
The pelvic floor and hip have to be stronger to counteract this increased force otherwise, this person may experience urine leakage or low back/hip/pelvic pain
Nervous System and the Pelvic Floor
For a long time, physicians and researchers thought tension in the pelvic floor was only related to physical or sexual abuse, which strikes me as a weird, illogical assumption. However, researchers connected electrodes to women’s pelvic floor muscles and trapezius muscles (the ones that are doing most of the work when it feels like your shoulders are up by your ears). They showed the women different types of movies. They found that pelvic floor tension is part of regular defense mechanisms/fight or flight responses.
According to Lauren Ohayon from Restore Your Core (can’t recommend her program highly enough by the way), feelings, presence, and sensation require a lot of energy from the body. Because of this our autonomic nervous system (what people talk about with fight or flight and rest and digest, though it’s a bit more complicated than that), uses sensation, memory, and past experience to guide what you will do. The system is designed for efficiency, so it is more likely to use tactics that are familiar over the ones that are the most functional. These adaptations influence breathing and postural patterns, emotional regulation, sensory awareness, and which parts of the body we connect to and which ones we avoid. When you have a quiet moment, lay down, try to sense your skin, muscles, bones, and organs individually. Notice which you can feel easily, which are difficult to perceive. Also note that the areas that are difficult to sense will only become easier when you are in an environment that feels safe.
The pelvic floor is one of the most sensitive and reactive parts of the body in its response to the nervous system. The pelvic floor is an anatomic part of you that correlates with the root chakra in yogic philosophy. A healthy root chakra is vital to our sense of safety and security. Echoing the traditional knowledge of the chakra system, the pelvic floor reflects a sense of safety more than muscle tone. When we don’t feel safe, it may manifest as pelvic gripping, numbing, and disconnection from sensation. Because of the numbing and disconnection, we often are unaware of the tension in our pelvic floors.
Creating a healthy pelvic floor requires stretching muscles, but it also requires slowing down, relaxation, and safety. The pelvis is a body structure that causes stimuli and responds to stimuli from head to toe. Though kegels have a role in caring for your pelvis, it's a small one. If you are curious about other ways to tend to your pelvic floor, you can find more specific exercises and movements below the paywall.
Activities That Support a Healthy Pelvic Floor
Deep Breathing
When we breathe deeply, it activates the parasympathetic nervous system and relaxes the pelvic floor. Lauren Ohayon from Restore Your Core describes this as Three Dimensional Breathing.
Rest your hands on the front of your ribs and try to breathe so that the chest wall expands forward and backward.
Place your hands on the sides of your ribs and try to expand your ribs from side to side
Place one hand near the top of your breast bone, the other on your lower ribs, then try to breath so your lungs expand from top to bottom.
Last, try to breathe so that your lungs are expanding in all three dimensions: front to back, side to side, and top to bottom.
Candle Breathing
Lauren Ohayon also discusses candle breathing as a technique for activating the reflexive core (your transversus abdominus muscles). Pretend you are blowing out candles on a cake. You should feel your abdominal muscles pull inward when you do this, but you might not initially. It may take some practice. You can try this standing, seated, or on hands and knees. Once you have mastered it, try to use it before any movements you make where core engagement is needed, like deadlifts and squats. When you use it for abdominal exercises like sit-ups or planks, it is important to know that if you are doing candle breathing, but still feeling bulging of the abdominal muscles, between the abdominal muscles, or the pelvis, then your abdomen cannot effectively manage that much pressure and you should do a less intense modification. If you’re curious about less intense modifications, please hit me up in the comments.
Muscle Release
External Pelvic Floor Release
Find a small ball (tennis ball, lacrosse ball). Place the ball somewhere between your sitting bones side to side and your pubic bone and tailbone front to back. Sit on it. This will help tight muscles release. If this is uncomfortable, you can decrease the load by leaning to one side or using a softer object. If those modifications are still painful, professional help from a pelvic floor physical therapist may be needed.
Internal Pelvic Floor Release
Just like you can massage painful muscles outside of the vagina, you can massage painful muscles inside the vagina. This can be especially helpful for people who experience painful sex. Learning proper technique for this type of massage from a professional is important to learn the anatomy of your pelvic floor muscles, how hard to apply pressure, and how long to apply pressure. You can create more tension instead of less if pressure is applied in the wrong location or too much pressure is applied.
Psoas Release
There are quite a few ways to perform a psoas release, but I will stick to the two simplest. Most people don’t feel much happening when they do this. I like to measure what happened by laying on the floor before and after the psoas release. Most people will feel like their mid and lower back is closer to the floor afterward than it was before.
Option 1: Use a yoga block, foam half-roller, sleeping bag, or pile of pillows. Place it under your pelvis. Lay there for 3-5 minutes. If desired, you can gradually scoot the top of your pelvis off of the yoga block, eventually landing on the floor.
Option 2: Use a yoga bolster, sleeping bag, or pile of pillows. Align the bolster so the bottom of it is at your bra line (the bottom edge of your shoulder blades for those who don’t wear bras). Lay down for at least 3-5 minutes. Relax. If you’d like to read about this release in more detail you can do so here.
Opening and Moving the Pelvic Floor
Internal and External Rotation of Hips
Internal and External Rotation of the hips are great ways to mobilize and strengthen the pelvic floor muscles. Many people suggest doing figure 4 stretch or pigeon pose to stretch in external rotation of the hip. If you have the mobility to do so that’s great, but for many people it forces them into a tucked pelvis which can destabilize the tailbone and/or lower back. That is especially true during pregnancy when connective tissues are more lax.
Half Happy Baby
Child’s Pose
Write the Alphabet With Your Butt
As we discussed a few weeks ago at the very end of the exercise video, you can write the alphabet with your sitting bones (the inferior pubic ramus). This moves the pelvic floor muscles in a lot of dimensions that it normally doesn’t.
Spinal Movements
Spinal Flexion/Extension
Cat Cow is a great way to move the spine in flexion and extension. When you do it, make sure you focus on moving each bone of the spine individually. It is really easy to skip over the chunks of the spine that don’t move well if you are not focused on it. For me, that is the thoracic spine (the upper back).
Spinal Side-to-Side Bending
My favorite way to do side bending of the spine is on the hands and knees. Simply peek toward your heels.
If you’d like to add internal and external rotation of the hips to the move, turn your feet toward the side you are looking toward.
Standing side-bends are a great way to strengthen your reflexive core. Before you start, do a candle breath until you feel your muscles pulling in, then bend to the side. If you feel bulging in your abdominal muscles or pelvic floor, don’t bend as far.
Spinal Twists
My favorite spinal twist is a simple one, lay on your right side with your knees bent. Put something under your head like a pillow or yoga block. Raise your left arm toward the sky, rotate your ribs toward the floor (don’t let your arm go farther than your ribs do). Enjoy.
Thread the needle is a great way to get spinal rotation from a hands and knees position.
To increase the degree of difficulty, build your balance, and get a really nice spinal and psoas stretch, you can add a side bend or twist to your lunges.
Stretch Your Shoulders
As I mentioned above, tight shoulders have a bigger than expected impact on our pelvic floors. Here are some ways to open your shoulders.
Hanging
Hanging is a wonderful way to care for your shoulders and stretch them out. In fact, there’s some research from a while back that showed that hanging relieved chronic shoulder pain in people who had shoulder impingement and rotator cuff injuries. Multiple people were able to cancel scheduled surgeries because of their improvement. You don’t have to be able to hang from a bar with your feet off the ground. You can start with your feet on the ground like this:
Gradually as your strength increases you can work toward longer times with your feet off the ground. You can also use tree branches, monkey bars or other things to hang from.
Internal and External Rotation
As you’ll see in the photos, my shoulder range of motion isn’t great right now, but the goal here is to rotate from the shoulder until your hands touch the wall. Then, rotate your shoulders so your hands touch the wall below you. If you have the range of motion to, try to pull your elbows off the wall. Experiment with how far you can move your arms if you let your ribs and spine lift off the wall versus if you don’t. Mainly do this exercise keeping your ribs and spine touching the wall because that isolates this move to the shoulder joint.
Abduction
For this move, rotate your hands so your thumbs are pointing toward the wall or the floor. You can do it standing or lying down. I like to do it standing because it is easier for me to feel when I’m lifting my ribs off the wall and bring them back down. Make snow angels with your arms (as far as you can without your ribs lifting off the wall).
Calf Stretch
The calf stretch is an antidote to the position we are always in in heeled shoes. That position shifts our knees forward, which shifts our hips forward, which shifts our upper back backward into a slouch, which tightens our neck and shoulder muscles, which leads to headaches. How’s that for interconnection? Stretching the calves influences the mechanics of every step you take and it can be easily modified to add hamstring and low back stretching to it. One of my favorite calf stretches is to place your toes on top of a half foam roller. You can use a rolled up towel or whatever you have handy. To make the stretch less intense step the foot on the floor backward. To make the stretch more intense step the foot on the floor forward.
Pelvic List
In our culture that wears shoes with heels and sits on our tailbones, our lateral hip muscles get really weak. Because we need our lateral hips for literally every step we take, this is a problem. In the pelvic list move, you are moving from your hip jutting out to the side to the hip being lined up back over the knee. I was going to make a video about this, but I can’t really top the instructions given by Katy Bowman in the video on this page.
Make Your Whole Body Movements Pelvis Friendly
Because the pelvis is so interconnected with everything else in the body, isolated exercises like kegels can’t accomplish what is needed to keep the pelvis stable, dynamic and responsive. Whole-body movements are needed. As biomechanist Katy Bowman notes, exercise is a very small portion of the movement our bodies were designed to integrate into our days. Here are a few of her suggestions for moving in ways that make your pelvis happy.
If you are experiencing symptoms of pelvic floor dysfunction like pain, prolapse, or incontinence, transition from high impact movements to low impact movements until that is healed. For example, if jumping rope makes you leak urine, that shows that your pelvic floor can’t manage the pressure in your abdomen currently. Continuing to keep things at a higher pressure can worsen pelvic floor tension.
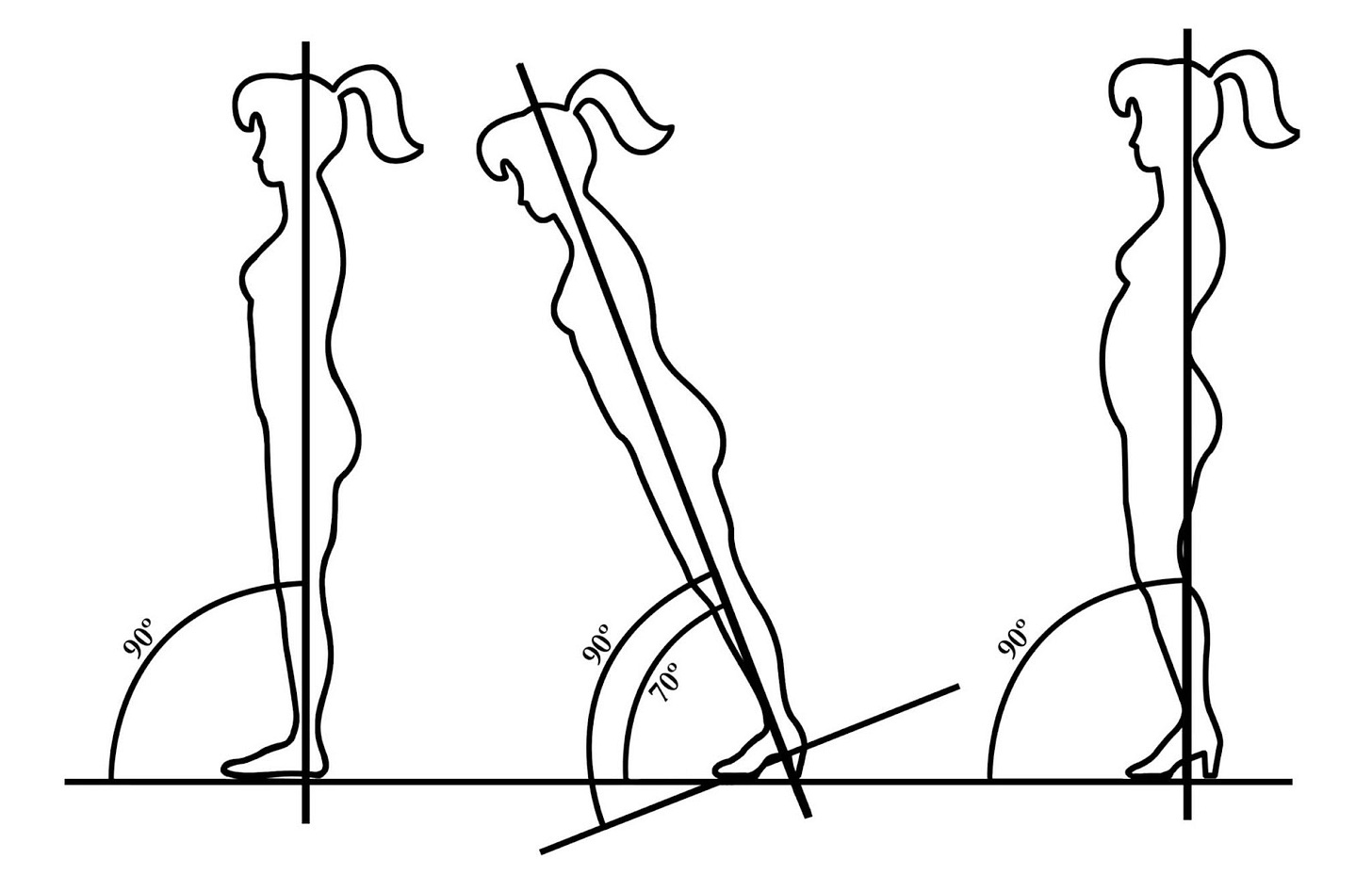
Bring your heels back to earth. Podiatrist William Rossi noted in his book Podiatry Management, “Any elevated heel automatically initiates an altered series of foot and body biomechanics.” This applies to high heeled shoes, but also men’s dress shoes or most types of running shoes. Here is a picture from Bowman’s book, Simple Steps to Foot Pain Relief:
You can see that in order to maintain an upright position in heels, the person’s knees and pelvis shift forward, the ribs flare upward and the curve of the spine is exaggerated.
Walk more, preferably outside. Walking helps the pelvis and glute muscles manage the constant load the weight of the organs places on the pelvic floor, by shifting and balancing that weight. If you must walk on a treadmill, walk slowly, uphill, so you can extend your hips and use your glute muscles as much as possible. Glute muscles are incredibly important for healthy walking and healthy pelvic floors. Happy to answer questions about this, but it might be worth a separate piece on its own.
Nearly every seat we find ourselves in encourages us to tuck our pelvis under and sit on our tailbones. This means the pelvic floor muscles don’t have to carry the weight of the organs. It also shortens the psoas muscle and leads us to tucking our pelves even when we are walking, which keeps us from engaging our glutes. See, it’s all connected. Sitting on the floor is better for the pelvis, but for most of us we can’t get into that untucked position all the way on the floor, so a few pillows or cushions might help.
Ultimately that children’s song about the foot bone connected to the knee bone was right on target, but in many ways the pelvis is kind of the hub of the wheel for our bodies. Despite how many words I’ve spilled about the pelvis, there are even more components to optimal pelvic floor function, like adding strength with sumo squats, Warrior 2 pose, and lunges, linking breath to movement and relaxing the jaw (try buzzing your lips for fun!). I’d love to hear your pelvis experience. What has hurt? What has helped? What do you want to know more about?






















I have hypermobile EDS so my pelvic area is even more prone to muscle and ligament stress. My PT has been so helpful in teaching me myofascial release, in addition to several of the techniques you describe. It really is the anchor of our body.